Category Archives: Movement Patterns
Nuts and Bolts of Fascia and Movement
Passion I’ve been doing bodywork for 23 years now. It sounds like a long time, but it always feels like there is so much more to learn. Just as I peel away the layers on soft tissue issues, I feel closer to the awe that is the human body. To me, it is like getting a fireworks show every time I think about its amazing power and resilience.
Currently, the two things that inspire me most are fascia and movement. And though both have been around since I started my journey, there is a thrilling amount of new information and study coming from each of these fields. My mentors are everything to me. I wouldn’t be where I am today without them. So in order to further explore my ideas about the resolution of hip pain, I think it is important to look at the sources I have found to be of benefit.
Fascia 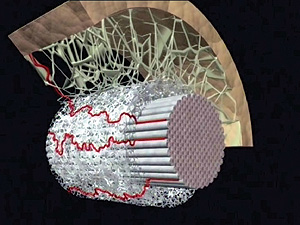 Despite the fact that fascia was first described over 100 years ago by, the founder of osteopathic medicine, Andrew Taylor Still, MD, the first international fascial conference was held only five years ago in 2007. With the advances in research methods and technology, most of what Dr. Still hypothesized about fascia, is now being proven.
Despite the fact that fascia was first described over 100 years ago by, the founder of osteopathic medicine, Andrew Taylor Still, MD, the first international fascial conference was held only five years ago in 2007. With the advances in research methods and technology, most of what Dr. Still hypothesized about fascia, is now being proven.
What is fascia? Fascia is a very densely woven covering that interpenetrates our organs, muscles, bones, nerves, and blood vessels. Of great significance, it is actually one continuous structural support that exists from head to toe without interruption. So truly an ankle sprain that doesn’t completely heal, can lead to headaches in your future if the fascia gets tight enough. Medicine prefers to look at the body in its parts, not in its connectedness. This is why as a bodyworker; fascia explains a lot of the clients that have fallen through the cracks in our healthcare system.
It took me until 2010 to have my own break out moment about the power of fascia. It was during a yoga workshop that I was introduced to the work of Tom Myers, the man behind Anatomy Trains. Leslie Kaminoff, of the Breathing Project, showed us a video dissection of the ‘deep front line’. And yes, just like in the movie Jerry Maguire, Tom Myers work had me at “hello.” It just tied together a lot of those loose ends. 
Movement Let’s move on to the new concepts in movement. Every time I turn around there is a new functional movement guru. Currently I am drawn to the work by Gray Cook and Kelly Starrett. My thought on why functional movement is sticking now vs. previously is because we are using these tools with our professional sport teams and getting results. They are showing that by doing a functional screening on these well paid athletes that they can predict their probability of injury. It’s funny how managers seem to prefer to pay for athletes that can stay in the game at their top performance vs. on the sideline.
Fascia and Movement relating to hip pain When I do an assessment on my clients with hip pain, I usually find a combination of both fascial and movement dysfunctions. The key for me is to address them in the proper order. If you don’t have the movement due to fascial tightness, I work to get rid of the restrictions before retraining their movement. If I find an unstable joint, I get it supported with tape or bracing and start strengthening at whatever level they can manage without pain. Even if I find fascial restrictions around this instability, I must be careful as taking any more stability away from an area may hinder my client more.
Hip pain Alignment check Here I find that the pelvis, sacrum and low back may be impacting the hip. Now I have to decide if the change is due to a one time trauma that has altered the position, or that a constant postural tension with fascial restrictions has led us to where we are today. Or the truly challenging and most common is a combination of both.
 Hip pain Movement Patterns The second biggest finding I have with hip pain is muscular imbalances in the hip, abdominal and pelvic floor muscles. My job is to figure out if the tissue is short and fascially restricted, or overactive and just on all the time and needs to be relieved of its overactive duties, or truly just weak.
Hip pain Movement Patterns The second biggest finding I have with hip pain is muscular imbalances in the hip, abdominal and pelvic floor muscles. My job is to figure out if the tissue is short and fascially restricted, or overactive and just on all the time and needs to be relieved of its overactive duties, or truly just weak.
“Maybe we are all cabinets of wonders.” ~ Brian Selznick
That’s it in a nutshell. I sense more details on hip rehab next time.
Is Your Story Keeping you from Your Best Health?
 Is your ‘story’ keeping you from your best health?
Is your ‘story’ keeping you from your best health?
Recently I received a call from a potential client who didn’t even offer me his name. He opened the conversation with who had referred him to me, and that he preferred to get in ASAP because of his pain. Since it seemed very important to him, I proceeded by inquiring about the nature of his pain. His response was that he has persistent pain in his shoulders, which he feels comes from a guarding pattern he can’t seem to change following a cervical spine fusion surgery.
Since his issue seemed really straight forward and I didn’t have space to fit him in that day, I recommended some other bodywork practices that may have immediate availability. But now the real story came out. “Would they know what to do with a fusion?” he asked. I find I am taken a little aback, as rarely do I get a referral for someone still on restrictions without getting a phone call from their practitioner or doctor. To clarify my questions, he stated that his surgery was over a year ago and he has been given the all clear by his surgeon to resume all his normal activities.
Here is the catch, and ultimately what may be creating an underlying holding pattern in the muscles of his shoulders. On his last visit, the doctor explained that on one view of his x-rays the bone looked as if it hadn’t completely filled in, but even with this information he was released from all his previous restrictions. So despite the wonderful hall pass he received, he leaves the doctors office in conflict. As he has heard that he is not whole, in fact still quite broken and fragile, with the fusion not being completely perfect. He also heard the words he is free to get back to his life as before. But now, he just may write his story that he is getting back to his life, but despite giving a year of his life to surgery, rehab and recovery, he still isn’t well.
He needs to believe that it is okay to not have a perfect x-ray at the one-year mark, and that the doctor feels very good with the outcome of his surgery even with these findings. And most importantly, it is okay to move on with your healing by editing this part of your story to mean that imperfect doesn’t mean broken. I hope he realizes this sooner rather than later, and gets back to being himself, and not his injury. I will know this is true if he calls again, and begins by giving me his name.
“Not everything that can be counted counts, And not everything that counts can be counted.” ~ Einstein
The Power of Looking Deeper
One of my favorite teachings reminds us that we already have everything we need to heal within us. This is not to say that modern or alternative medicine isn’t necessary. However, just hold this thought, tangibly in your hands, for a moment and think about how powerful it really is.
As a body worker, I would be out of a job if we were always capable of figuring out exactly what it is we need. My observation, over the years, is that many people need a clearly definable and fixable injury or illness for them to move forward in their recovery.
But what about the thing that just hurts sometimes, or despite a diagnosis and sound treatment plan, it remains present and quite annoying in your life. What if that tension you hold is deeper than your annoying boss, your daily grind or a past physical trauma?
We start our patterning really early. Some believe from the day that we take our first breath. I don’t know about you, but I can’t remember how easy it was or wasn’t to breathe, or to crawl, or to walk. But all of those skills initiate our internal wiring. It is completely subconscious, but still there never the less. Based on our life experiences, we learn to keep certain muscles chronically tight, and our joints compensate around this imbalance. Luckily, given the right attention to detail, this can be restored.
“Life is the sum of all your choices.” ~Albert Camus

 Level 1 Certification Complete
Level 1 Certification Complete